Streamlining Vision Screenings for People with Diabetes in Indonesia
Many people don’t realize that diabetes affects the eyes. But if you have diabetes and are blind to this truth you could lose your sight.
Diabetic retinopathy is a complication many with diabetes face, particularly if the disease is not well managed. Chronically high blood sugar can damage small blood vessels in the back of the eye, distorting vision. A leading cause of preventable blindness among working adults, it can be treated if identified early enough. In 2000, the number of people with diabetes in Indonesia was estimated at 8.4 million. This number is expected to almost triple by 2030.
Annual eye exams for people with diabetes is not routine practice in Indonesia like it is in countries like the United States, and the process to access care if something is amiss is dizzying. At monthly visits at a primary health center clinic vital signs are checked, blood is drawn, and a consultation occurs with a general practitioner. If concerns are raised, the GP refers the patient to a district hospital for a consultation with an endocrinologist. If an ocular condition is suspected, the person will be referred to an ophthalmologist. But at district hospitals, ophthalmologists don’t often have access to retinal cameras, so patients may be referred to a third hospital for a definitive diagnosis before then being sent back to a district hospital for laser treatment.
In this system, patients only reached the point of diagnosis if something obvious was wrong. But early diabetic retinopathy—when the disease is most treatable—shows no symptoms. This system meant less than 20% of people with diabetes were seen by an ophthalmologist. HKI saw a need for change.
“As many as one in three people with diabetes may develop diabetic retinopathy, which would lead to a public health emergency in Indonesia,” says Country Director Prateek Gupta. “We saw an opportunity to work with the government and the hospitals to update systems to reduce preventable blindness.”
In 2009, a hospital-based screening program was established in Jakarta. People with diabetes visiting the endocrinology clinic would have retinal photographs taken, and the images would then be transferred to the ophthalmology department. Any patients with diabetic retinopathy would be referred to an eye clinic for care. The process was then replicated in Bandung and Yogyakarta, two cities believed to have many people with diabetes.
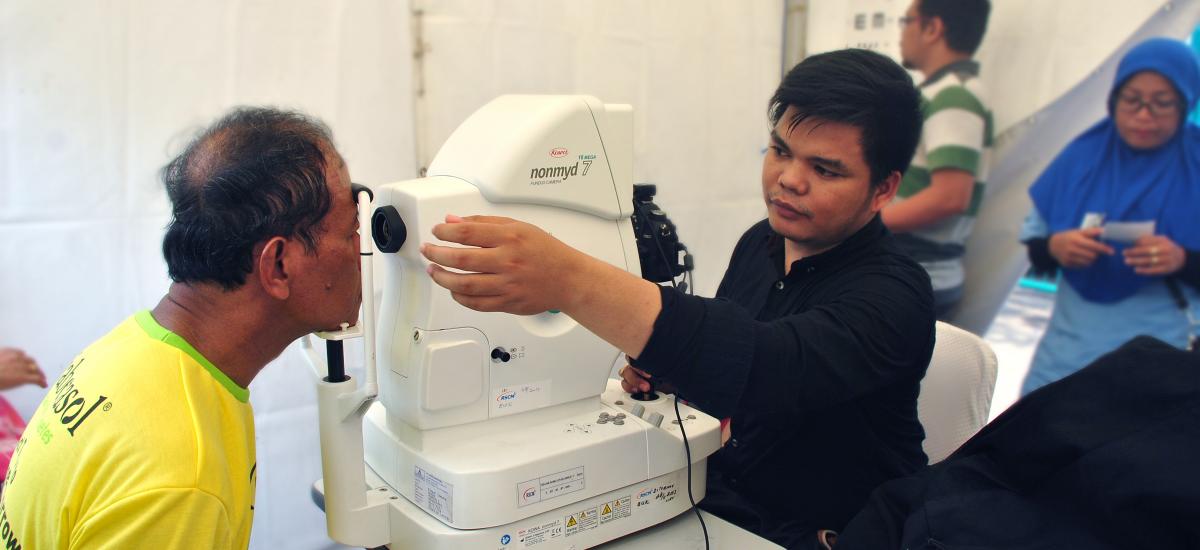
In an effort to reach more patients and raise awareness, teams tested a new model in Jakarta that revealed valuable information that could ensure greater future success. In some primary health centers, a procedure for screening using fundus cameras: microscopes with attached cameras. Retinal photographs were taken identify the presence of diabetic retinopathy or other undetected conditions; images that were unclear or raised concerns earned patients referrals to a district hospital. In other primary health centers, education was provided.
Surveys of patients following both efforts revealed a lack of awareness of the need for eye care. The first method proved more effective in addressing the need for care, as the fundus cameras enabled greater patient screening at the earliest touch point. HKI also learned that patients simply told to visit a hospital were unlikely to follow through, but written referrals enabled reimbursement.
Since HKI began working with the government to address diabetic retinopathy, 10,000 patients have been screened and almost 2,000 treated. Perhaps more importantly, by building the capacity of the healthcare system and the professionals working in it, these efforts set the stage for more effective care to come.
“We look forward to working with our partners in the Indonesian government and at the health facilities to identify new models for screening and treatment and expanding access to vision-saving care,” says Gupta.




