
3 Things We’re Optimistic About in 2021
“Optimism is the faith that leads to achievement. Nothing can be done without hope and confidence.” – Helen Keller
2020 was a challenging, sad, and scary year. The stroke of midnight on January 1, 2021, did not wipe the slate clean. However, guided by the fierce optimism of our co-founder, Helen Keller, who overcame seemingly insurmountable obstacles to live a life of purpose and service, we choose to side with hope.
The new decade dawned with some promising advances. Foremost in people’s minds is the coronavirus vaccine, but we have seen significant progress in other areas as well. With grit and resilience, we look bravely towards these opportunities. We focus on what we can do, and we poise ourselves for action to improve the lives of the people we serve. Here are three things that we are hopeful for in 2021:
1After months-long pauses due to COVID-19 safety concerns, programs to deliver life-saving vitamin A supplements and life-changing drugs are now back in action across West and East Africa.
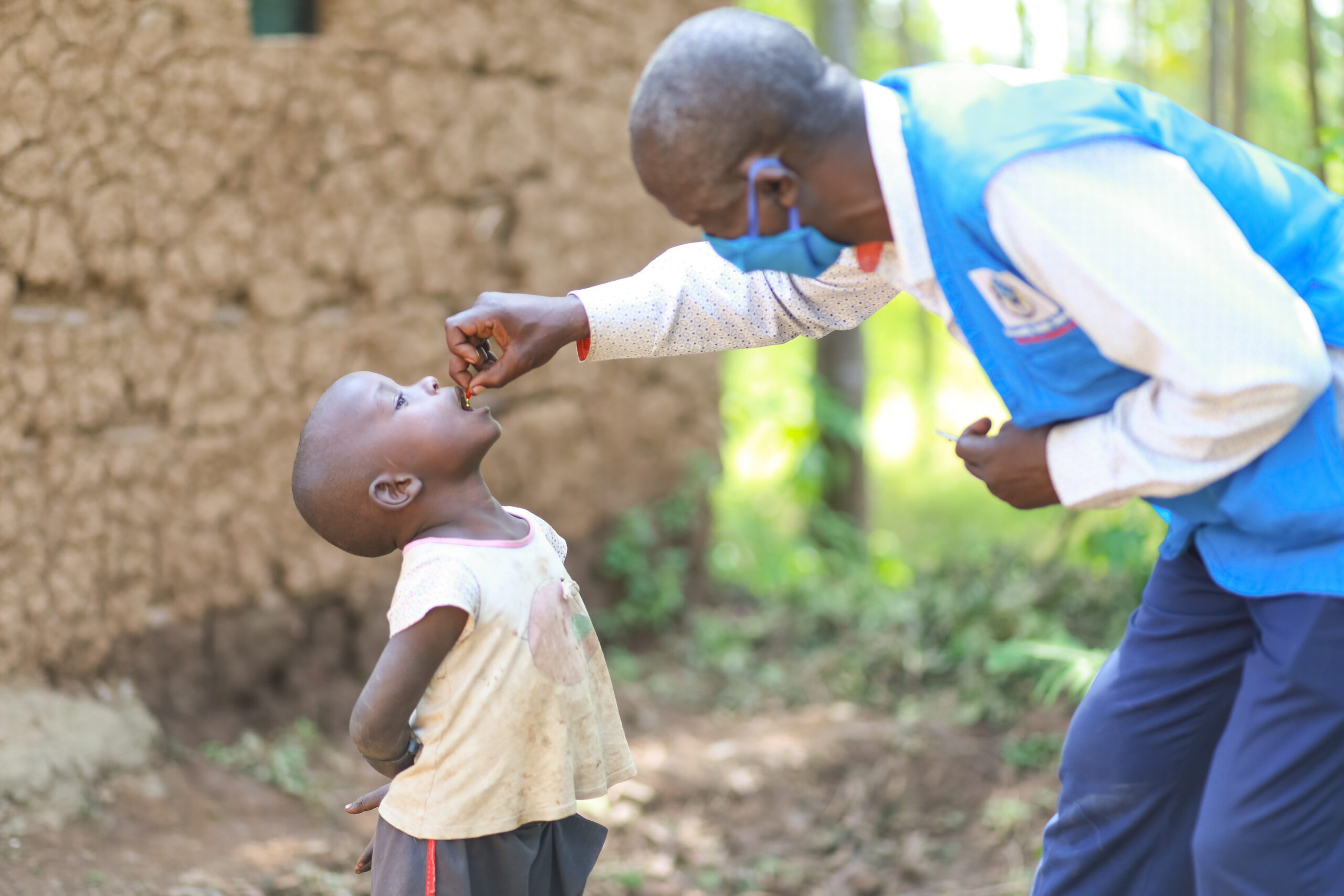
Vitamin A supplements strengthen children’s immune systems and can mean the difference between surviving and succumbing to common childhood illnesses. (Two doses of vitamin A supplementation per year can reduce childhood mortality by almost a quarter.) Medicines that prevent and treat parasitic and bacterial infections, meanwhile, save millions of people from debilitating and disfiguring “neglected tropical diseases” (also known as diseases of poverty) like elephantiasis and trachoma each year. When COVID-19 first hit, we had to stop vitamin A and neglected tropical disease treatment. This prevented spreading the disease, but it put millions more people at risk for the malnutrition, disease, and death that the campaigns prevent.
Thankfully, the story didn’t end there. We knew we had to get treatments out, as early as possible, but without putting people at risk. Alongside governments, in-country partners, and other stakeholders, Helen Keller Intl helped to develop rigorous safety protocols that protect both health workers and community members from coronavirus during treatment. Campaigns are now back on track, including making up for lost time. We will continue to work with added safety measures until the pandemic ends.

2 The world is moving towards a simpler and more effective way of managing malnutrition. While hunger is on the rise as a secondary effect of COVID-19, so, too, will be the number of people successfully treated for it.
The World Health Organization’s longstanding protocol for management of malnutrition is three-pronged. After community health workers diagnose children with malnutrition, cases of moderate malnutrition are treated at the community level, and cases of severe malnutrition are referred for treatment at health centers. Children with severe malnutrition without complications receive out-patient care from the health centers – requiring them to travel back to the center once a week. Children with complications (for example, being unable to swallow water or breastfeed) receive in-patient care.
Over time, drawbacks to this approach became apparent. Many parents of children who are referred for treatment at health centers do not have the money or the means to travel once a week. Thus, children miss appointments and fall through the cracks. The COVID-19 pandemic aggravated this issue further. Parents were afraid to go to health centers for fear of the virus, so children went untreated.
Because of COVID-19, Helen Keller Intl is pushing for a fast shift to a new, simpler, and scientifically proven protocol:
- Diagnosis of malnutrition and its severity level are determined with a specially marked strip that is wrapped around a child’s mid-upper arm, as well as observation of related conditions, such as swelling in the face and extremities. (With the old method, assessment of malnutrition also typically requires additional body measurements, including height and weight, which are difficult and time-consuming to obtain.)
- Health centers only treat complicated severe malnutrition and leave management of uncomplicated severe malnutrition to community health workers, who have received appropriate training. The community health workers treat cases of both moderate malnutrition and uncomplicated severe malnutrition with the same products – a combination of peanut butter, milk powder, and vitamins – dosed according to the child’s condition.
The result of the simplified protocol is a decreased burden on health facilities and an increase in the number of children who receive a full course of treatment. And that’s very encouraging news.

3 We are on the brink of eliminating lymphatic filariasis, which impacts the most undernourished and underserved areas of the world.
If you’ve never heard of lymphatic filariasis, that’s because it is not seen in economically better-off countries. This “neglected tropical disease” – an umbrella term for about 20 debilitating communicable diseases that mostly impact people living in poverty – leads to extreme swelling of the arms, legs, feet, and genitalia. Like malaria, lymphatic filariasis is spread by mosquitoes. Over one billion people around the world are at risk of contracting it.
Thankfully, the public health community has all the tools we need to prevent this disease. Simple treatment and prevention campaigns at the community level have already made a huge impact. It takes between five and seven years of campaigns to eliminate lymphatic filariasis as a public health problem in any given region. We’ve been working in countries including Mali, Burkina Faso, Niger, and Sierra Leone to beat this terrible condition. We have reason to believe that we will soon succeed.
We are reaching more people than ever before with treatments to eliminate and control neglected tropical diseases. This has led to a steady drumbeat of countries – 33 since 2012 – that have eliminated at least one neglected tropical disease. Helen Keller is proud to play a key part in this work.




